Plantar heel pain / plantar fasciitis – Your 8 incredible protective mechanisms
Why all the fuss about heel pain I hear you say? Well unless you’ve had it, I guess you won’t really know. Those who suffer from it describe it as:
Hell Debilitating Painful Torture
Excruciating Crippling Depressing
Relentless Annoying Exhausting
Frustrating Stabbing Horrendous Agony
But why does heel pain affect us with what appears to be such intensity? To understand that, we have to realise how important our heels are to us, and get to grips with their structure that makes them so unique.
Our heels are generally the first point of contact with the ground when we walk. In fact, one of the stages of foot function is called the “heel rocker”. Now that’s not some new rock star who enjoys wearing heeled boots to complement their leather jacket. No, it’s the first stage of the stance (weight-bearing) phase of gait (walking), which is then followed by the “ankle rocker” and the “toe rocker”. As the part of the body that makes that initial contact with the ground, and bearing in mind Newton’s third law that states “For every action, there is an equal and opposite reaction”, our heels have to take an awful lot of impact force. That force is actually more than our body weight and can be substantially more depending on what activity we are doing. So imagine all of your body weight (and more) focussed onto an area smaller than your ear! That is definitely going to get damaged if it isn’t protected or ready for it.
Fortunately, there are some mechanisms that human design has incorporated to help make sure our heels (and feet) don’t break as they load throughout gait and other activities. Here are 8 of those mechanisms, together with some of the things that can go wrong with those parts of our body:
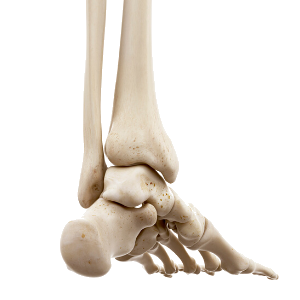 Brilliant bone
Brilliant bone
Our heel bone, also known as the calcaneum or os calcis, is the largest bone in the foot. Its trabecular structure is such that it is very strong, yet lightweight. It is subjected to both compression forces from the ground (possibly dampened by our footwear) and tractional forces from the soft tissues that attach into it (see below). The bone can get damaged in several ways generally resulting in either bone stress reaction / oedema, or stress fracture, or a truly broken heel bone (calcaneal fracture such as “lovers’ fracture”).
 Luscious layers of muscles
Luscious layers of muscles
There are 4 distinct layers of muscles under the soles of our feet, some of which insert into the heel bone and contribute to the tractional force on it already mentioned. These muscles are designed to help control the way our foot functions, including helping to manage the loading forces. The area where a ligament or muscle (via a tendon) inserts into a bone is called an enthesis. That can get damaged (enthesopathy) or inflamed (enthesitis). A weakness of the intrinsic muscles of the foot occurs quite easily due to the flat, hard surfaces we generally walk on.
 Awesome arch architecture
Awesome arch architecture
The structure of the foot is quite amazing. During walking (amongst other weightbearing activities such as running, dancing, cycling etc), it transforms from a mobile adaptor (through pronation) to absorb impact forces and transfer weight over uneven ground, before becoming a rigid lever (through supination) to push off with. The medial longitudinal arch is an important part of this and it sometimes doesn’t function as well as it possibly could. You may hear the term excessive pronation linked to heel pain and plantar fasciitis, but this is a misnomer that is perpetuated partly because it makes for simple sales pitches (of things like stability control running shoes and orthotics). It is important to understand that a flattened foot arch does not necessarily mean there is anything wrong with you, and the same goes for a high arched foot.
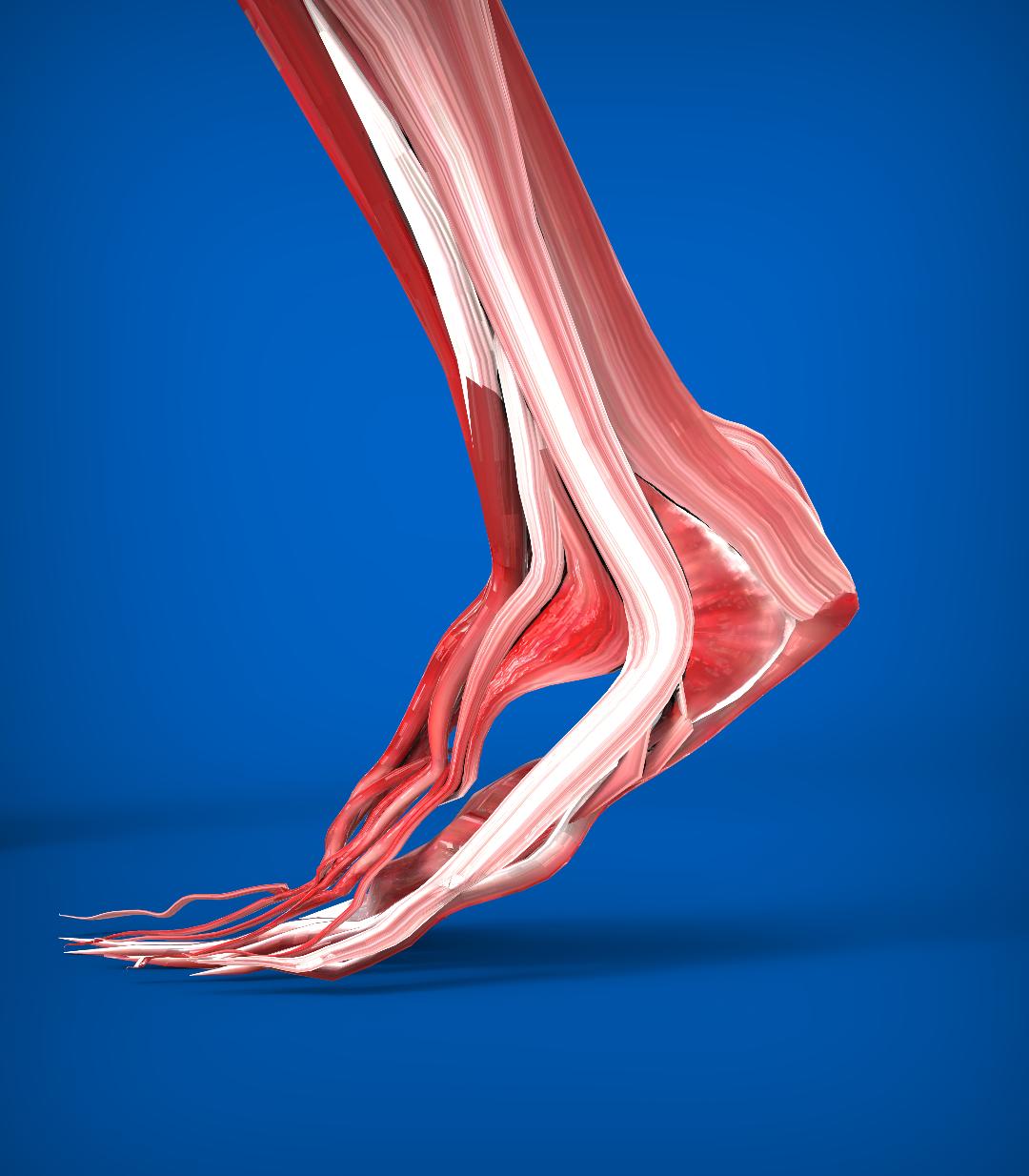 Fantastic fascia
Fantastic fascia
The plantar fascia is a structure that doesn’t really know if it is a ligament or a tendon as it has properties & functions that could apply to both of those soft tissues. It runs from underneath the heel bone to the ball of the foot. It helps to maintain the structure of the arch in our foot, it stretches to absorb loading forces, and stores up elastic tension as part of the Windlass mechanism, which helps to spring us forward as we walk. When damaged, it is all too often referred to as plantarfasciitis (inflammation), whereas in lots of cases it is plantarfasciosis (degeneration) that is the actual problem.
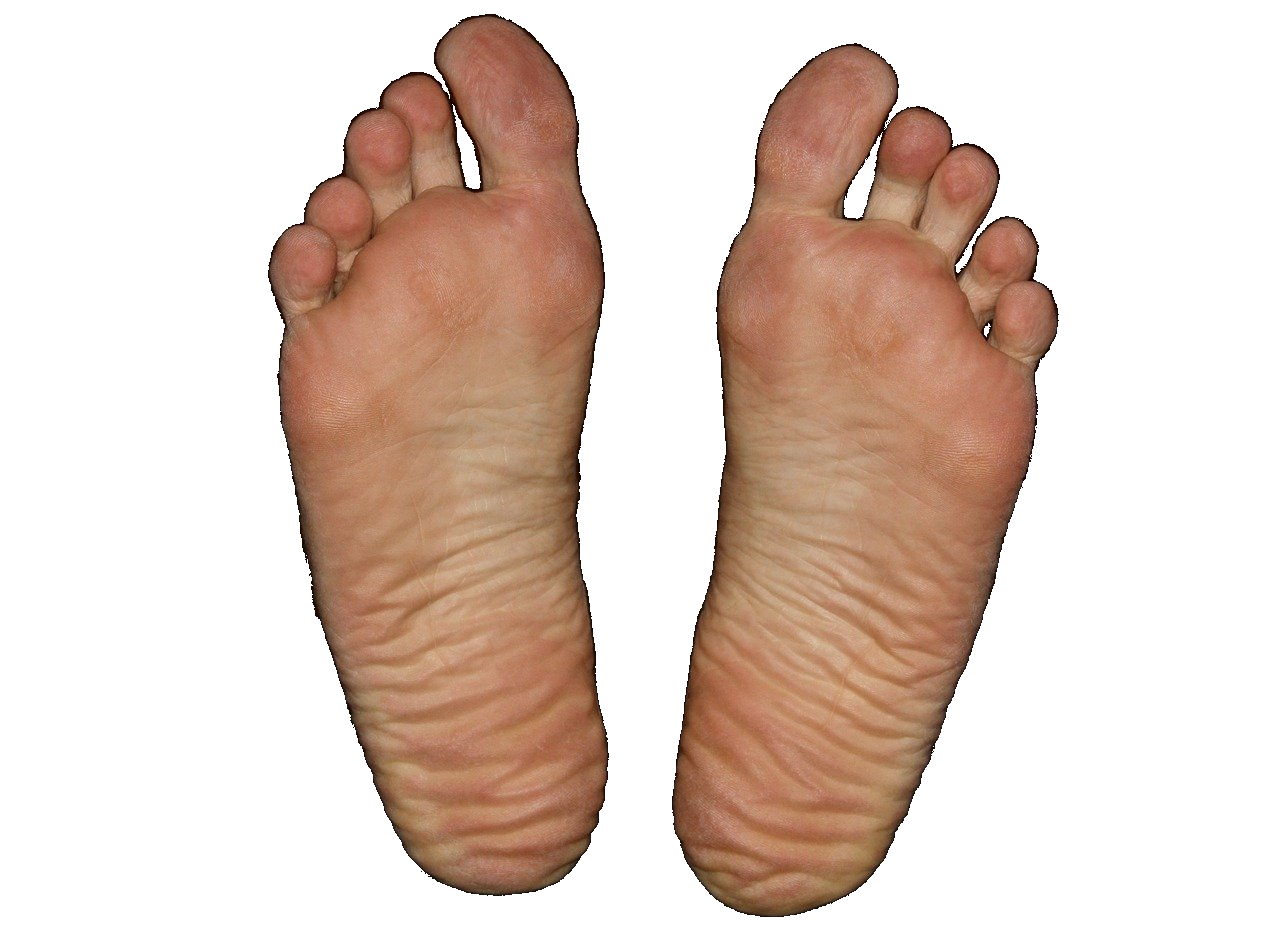 Fabulous fatty heel
Fabulous fatty heel
Directly under our heels is a fat pad which is specifically designed to attenuate shock. It’s the one part of your body you really don’t want to lose fat from if you are dieting (although I’m not sure if that is even possible!). It should be thick and dense, but lots of things can go wrong with it. If that happens, we refer to it as heel fat pad syndrome, but this could actually be due to atrophy / wasting / thinning / displacement of the pad, or inflammation / bruising of it. Repeated steroid injections can cause real problems with the heel fat pad.
 Bouncing bursa
Bouncing bursa
Bursae are fluid-filled sacs found deep in the soft tissues often next to the bone. Synovial bursae are generally designed to afford protection and/or improve the function of soft tissues such as tendons from the harder tissue of bone. For instance, the retrocalcaneal bursa sits between the calcaneum and Achilles tendon. However adventitious bursae usually form because of repeated pressure or shearing. So, if you imagine a small water balloon under your heel, it would serve the function of protecting the heel from impact forces. But it can get irritated creating a plantar calcaneal bursitis (also known as “Policeman’s Heel”).
Amazing Achilles heel
The dictionary defines this as “A weakness in spite of overall strength, which can lead to downfall”. Well, this is certainly true for heel pain, which of course you would expect as this is the part of the body where the phrase originated from in Greek mythology. Our Achilles tendon inserts into the heel bone at the back of and extends upwards to meet the calf muscles. When a tendon (and its corresponding muscle) shortens, it is known as concentric contraction. When they lengthen under load, it is known as eccentric contraction. Insertional Achilles tendonitis (or tendinosis) be classed as heel pain, but you can also get other types.
Magnificent muscles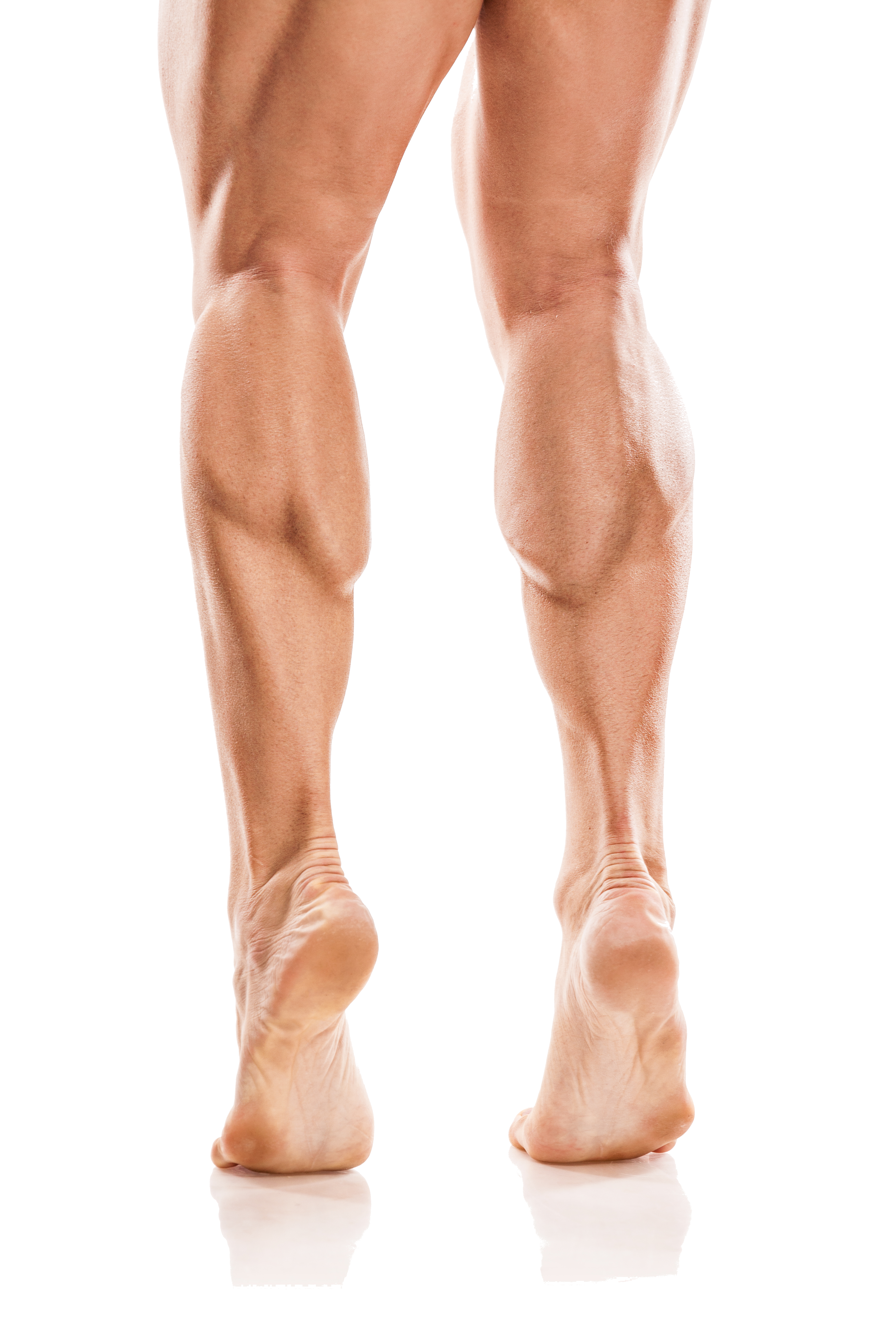
Muscle is an incredible structure. It can generate power to lift over 1000kg (for the strongest weightlifters) or run 100m in less than 10secs (for the fastest runners). But did you also know that muscle fibres themselves have the ability to transform to be able to absorb shock? And our calf muscles (known as the “triceps surae”) do that on every single step we take. Crazy eh? So problems with them (such as tightness / weakness / imbalance / atrophy / wastage) can contribute to heel pain, as well as those things affecting other muscles, especially our core ones. This is why strength & exercise is so important to the resolution of plantar fasciitis.
These complex structures and their possible associated problems show that not all heel pain is plantar fasciitis. If you have heel pain or know anyone who does, then make sure of an accurate diagnosis. Treating the wrong condition in the right way won’t achieve resolution. Neither will treating the right condition in the wrong way. The path to success with heel pain is to treat the right condition in the right way. This is why good Podiatrists are your best port of call. They have spent at least 3 years learning about feet and related problems at Diploma (no longer available), Degree, Masters, or Doctorate level. So in most cases, they know more about feet than any other health care professional, so they are best placed to help fix feet. If you don’t get the answers you need from the first one you see, then talk to another one. There will be a Podiatrist somewhere who is ideally suited to you and your needs. Remember #PodsHealHeels and #PodsFixFeet.
Follow this link if you need further help:
