Treatment of Plantar Fasciitis / Heel Pain #podshealheels
 Welcome to the last in a series of 3 articles about plantar fasciitis that I hope will help you understand the processes involved in achieving resolution of this often frustrating and sometimes debilitating foot condition. In this article we will look at treating the problem.
Welcome to the last in a series of 3 articles about plantar fasciitis that I hope will help you understand the processes involved in achieving resolution of this often frustrating and sometimes debilitating foot condition. In this article we will look at treating the problem.
To keep terminology simple, I will use the label “heel pain” even though sometimes symptoms may vary from just pain and they may be located adjacent to the heel or further from it. For more information on the many possible diagnoses, please see the previous article in this series.
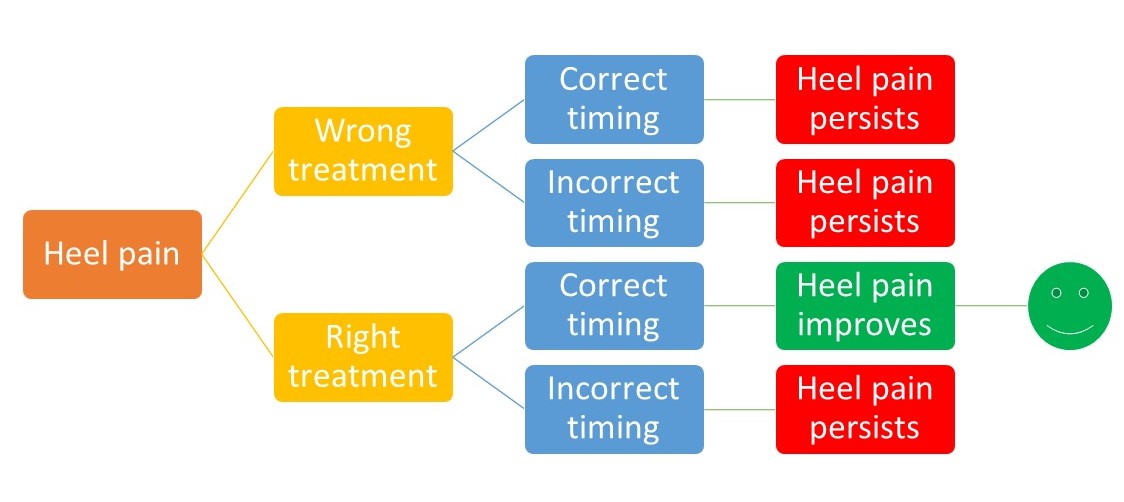
 I reckon there are more treatment options for heel pain than the 57 varieties of Heinz, the world-famous manufacturer of baked beans. The reason that so many treatment options have developed over time, is because there is not one single guaranteed fix for the problem. In part this is due to people not being diagnosed correctly, and so embarking on inappropriate or ineffectual treatment regimes. Additionally, the following simplistic flowchart applies for every type of heel pain and every possible successful treatment:So getting the right treatment at the right time is the only way to achieve resolution. As a result of this, there will be some success borne from luck (in the simple example above the odds of improvement are 25%). Note that as the condition improves the treatment may need to change, and the timing of that change is important too. That then creates a much more complicated flowchart, and the odds of success from luck become much less, which is why an individualised treatment plan following indepth assessment and accurate diagnosis is essential to achieve complete resolution of symptoms.
I reckon there are more treatment options for heel pain than the 57 varieties of Heinz, the world-famous manufacturer of baked beans. The reason that so many treatment options have developed over time, is because there is not one single guaranteed fix for the problem. In part this is due to people not being diagnosed correctly, and so embarking on inappropriate or ineffectual treatment regimes. Additionally, the following simplistic flowchart applies for every type of heel pain and every possible successful treatment:So getting the right treatment at the right time is the only way to achieve resolution. As a result of this, there will be some success borne from luck (in the simple example above the odds of improvement are 25%). Note that as the condition improves the treatment may need to change, and the timing of that change is important too. That then creates a much more complicated flowchart, and the odds of success from luck become much less, which is why an individualised treatment plan following indepth assessment and accurate diagnosis is essential to achieve complete resolution of symptoms.
 The more treatment options available and the more the understanding of those, the better the chances of achieving symptom improvement / resolution. If the only tool you have in your tool box is a hammer, then all your problems begin to look like nails. The more tools (treatment options) you have available, the more the specific problem (diagnosis) can be addressed, and this is where good Podiatrists come in for treating heel pain. They will be able to offer some or all of the following at the right time for the right condition to fix foot problems including heel pain / plantarfasciitis:
The more treatment options available and the more the understanding of those, the better the chances of achieving symptom improvement / resolution. If the only tool you have in your tool box is a hammer, then all your problems begin to look like nails. The more tools (treatment options) you have available, the more the specific problem (diagnosis) can be addressed, and this is where good Podiatrists come in for treating heel pain. They will be able to offer some or all of the following at the right time for the right condition to fix foot problems including heel pain / plantarfasciitis:
Strapping therapy – We tend to use this for acute presentations of plantar fasciopathy and/or fat pad atrophy. Personally I tend to use a progressive strapping programme over a period of 3 weeks and this provides significant improvement quickly, whilst gradually increasing the stretch on the plantarfascia.
 Load modification – By altering the load through the damaged tissue, symptomatic relief generally follows if done at the right time for the right condition. This may be through weight loss, activity modification, change in footwear, support socks, and the use of Gel Heel Cushions and/or functional foot orthoses (orthotics).
Load modification – By altering the load through the damaged tissue, symptomatic relief generally follows if done at the right time for the right condition. This may be through weight loss, activity modification, change in footwear, support socks, and the use of Gel Heel Cushions and/or functional foot orthoses (orthotics).
Orthotics – These are worthy of a separate mention as the term is often used alongside plantarfasciitis. To be clear, saying ‘wear orthotics for heel pain’, is like saying ‘take tablets for chest pain’. Without a diagnosis and understanding of what the orthotic or tablet needs to do, then how do we know what prescription is required. Orthotics should be prescribed in the same way that tablets are – materials properties, known interaction with the body, the dosage required for maximum effect, the length of the course of treatment, awareness of the side effects, and a review with the prescriber if symptoms persist for a possible change of prescription. On top of that there are cost implications that may influence the choice between the different types such as:
- Over the counter (OTC) or off-the-shelf (OTS) orthoses also known as stock orthotics
- Semi-bespoke orthoses which includes chairside insoles and heat-mouldable orthotics
- Bespoke orthoses which are casted orthotics made specifically for the individual
Electrotherapy – In the past ultrasound therapy was a mainstay of treatment but it has been shown that results with it aren’t much better than placebo effect. Low level laser therapy is similar, but the electrotherapy that achieves the best results and is advocated by the National Institute of Clinical Excellence for the NHS is shockwave therapy of which there are different sorts and different prescriptions, just like with orthotics. The same therefore applies – machine properties, known interaction with the body, the dosage required for maximum effect, the length of the course of treatment, awareness of the side effects, and a review with the prescriber if symptoms persist for a possible change of prescription. On top of that there are cost implications that may influence the choice of treatment regime.
Mobilisations / Manipulations – These can help with soft tissue and joint movements to reduce strain on the plantarfascia. More and more podiatrists are making use of these techniques to help their patients.
Rehabilitation programmes – By stretching (possibly with help from a night-resting splint) and strengthening appropriate tissues with gradually increasing load, then the body’s cells repair and regenerate to ensure long-term resolution of symptoms. This is where patients have to do the work every day, and avoidance of it is the main reason for prescribed treatment plans not being as effective as they could be. In addition regular use of ice and elevation, or heat and massage at the right stages of healing can be useful.
Steroid injections – There are various injections that we use in specific situations to give relief from heel pain.  They are not indicated nor effective in all cases, and when used as the only treatment, they rarely provide long-term resolution. Some injections are painful but pain-free techniques can be used by those trained to do them properly. Guided injections are thought to be more accurate in their placement of the steroid to reduce inflammation in a specific ‘hot-spot’ location.
They are not indicated nor effective in all cases, and when used as the only treatment, they rarely provide long-term resolution. Some injections are painful but pain-free techniques can be used by those trained to do them properly. Guided injections are thought to be more accurate in their placement of the steroid to reduce inflammation in a specific ‘hot-spot’ location.
Others – Some Podiatrists make use of acupuncture to help ease symptoms, and referral for platelet rich plasma injections or plantarfascia release surgery are also possible if required.
 Review – This is an important part of a treatment programme to ensure progression to full resolution of symptoms and return to desired activities. A good review revisits, adjusts, plans, and supports the patient in the management of their heel pain.
Review – This is an important part of a treatment programme to ensure progression to full resolution of symptoms and return to desired activities. A good review revisits, adjusts, plans, and supports the patient in the management of their heel pain.
By following all of the assessment, diagnosis, and treatment process for heel pain (“plantar fasciitis”), the condition should progress to complete resolution. In the same way that ‘Beanz meanz Heinz’ then ‘Plantarfasciitis means Podiatrists’. Nearly all of the above treatments are available from Jonathan Small, Lead Podiatrist at Health First Foot & Gait Clinic in Southam, Warwickshire, and Theorem Health & Wellness in Alcester, Warwickshire. Remember that Podiatrists are the Foot Specialists – #PodsHealHeels and #PodsFixFeet.
www.facebook.com/healthfirstsoutham
01926 811272 health1first@aol.com
www.theoremhealth.co.uk/podiatry
Review on Yell from JoW-254
“Plantar Fasciitis treatment – Specialist advice from a highly knowledgeable and skilled professional- bridging the gap between podiatry and physio for successful outcomes.”
