How To Cure Fungal Toenails (Onychomycosis)
You’ve probably seen the adverts on TV trying to sell cures for fungal toenails – those nails which are yellow, thickened, crumbly, and sometimes painful. That shows you how common the problem is when it is worth the pharmaceutical companies spending money advertising their products on TV. And it is common, very common – depending on which research papers you read, it affects up to 1 in 4 of the general population and 1 in 2 or less as we get older.
The problem with the treatments they advertise on TV is that they generally have low chances of success if the degree of fungal infection is extensive in terms of the amount of a nail that is infected and also the number of nails infected. However, the chances of success can be greatly increased with 6 simple interventions:
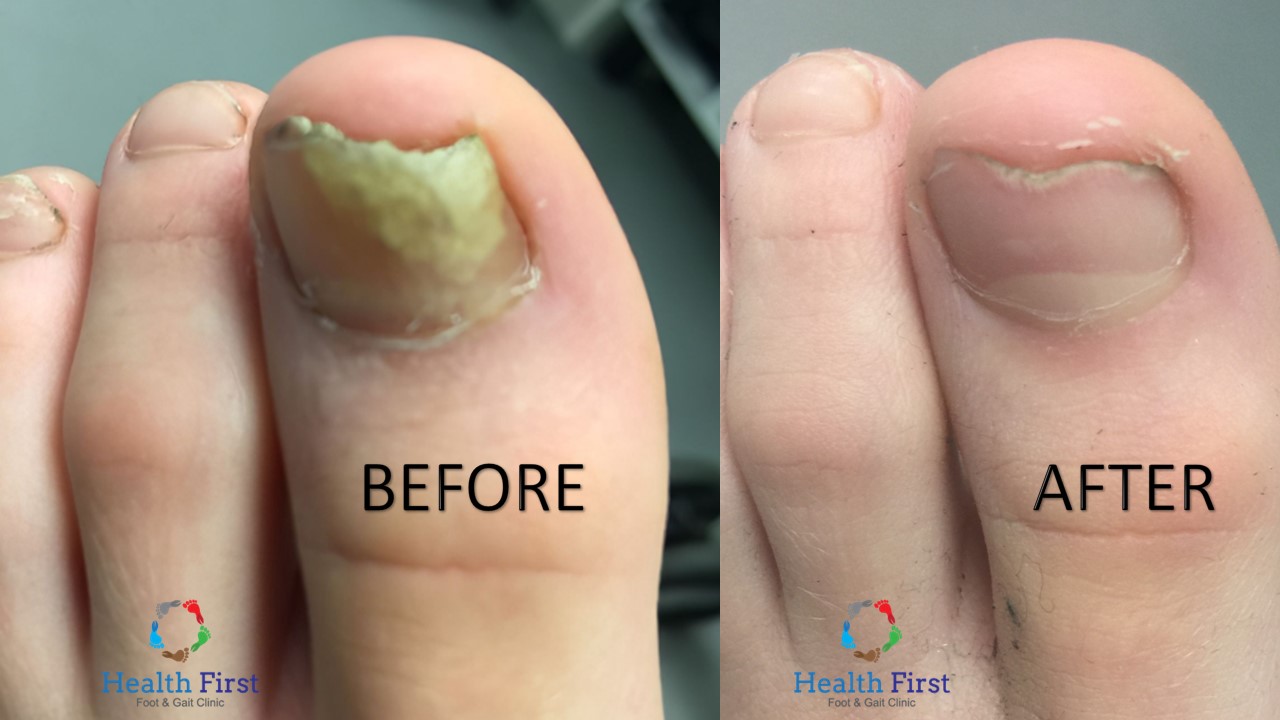
Treating fungal nails
TESTING THE NAILS
This is to confirm that you really have a fungal infection, as there are other medical conditions that can cause the nails to appear different eg. psoriasis, nail bed trauma, poor circulation, etc. It used to be the case that testing took several weeks and was fraught with false negative results (and still is the case for NHS care). However, at some private clinics like ours, there is now the equivalent of a lateral flow test for fungal infections (both nail & skin) with highly accurate results available in just 5 minutes.
REMOVING INFECTED PARTS OF THE NAIL(S)
Depending on the extent of the infection, this can either be done professionally & gently using drills, scalpels, and nail clippers; or it can be done more aggressively with no pain under local anesthetic (part or full nail removal). The less infected nail tissue remaining, the more chance of success with topical antifungal treatments.
ENABLING ANTIFUNGAL AGENTS TO REACH THE NAIL BED
Professional thinning of the nail or drilling of holes through the nail plate (fenestration / Lacuna), or part/full nail removal (described above) will help ensure that antifungal paints & sprays can reach the nail bed to eradicate any fungal infection there. The only exception is if the antifungal agent is in tablet form that you take orally, but note that NHS guidelines advise that you need at least 3 nails fully infected to warrant this sort of treatment.
TREATING FOOTWEAR
Fungal infection loves warm, moist environments such as is found inside socks & shoes. Therefore it is important to ensure any fungus is treated inside those, and today’s low-temperature washes just don’t do the trick. Footwear (both socks & shoes) should be treated with antifungal sprays daily, and/or can be sanitised in a special Klenz machine such as the one we have available in reception at our clinic.
TREAT THE SKIN
Nearly always, fungal infection of the nails is concurrent with fungal infection of the skin, and in the vast majority of cases, skin infection leads to nail infection due to the migration of the fungal spores under the nail plate. It is therefore important that the skin is also treated as this will help to avoid the recurrence of nail infection once resolved.
BE CONSISTENT WITH TREATMENTS
Fungal infection can require many months of treatment, with regular and continued removal of infected parts of the nail(s) to enable the antifungal agent to reach the nail bed. However, if the nail has been removed completely, then further removal should not be required. Please note that there is always the option when removing a nail for it either to be permanent or to allow a new nail to regrow over time, hopefully without fungal infection if treated properly.
Fungal nail infection (proper name = onychomycosis) is one of the most common things we help patients within our clinic here in Southam. We offer low, moderate, and high success rates depending on which treatment option you choose. So if you have any toenail problems, call us to make an appointment on 01926 811272 or visit our easy online booking system.
Take a look here, to learn more about fungal toenails.
Jonathan Small, Lead Podiatrist, Health First Foot & Gait Clinic | Southam.